H.R. 1 & Nursing Doctorates: Complete Series
Confused about whether nursing degrees are still "professional"? This 5-part series breaks down what Trump's H.R. 1 actually changes, and what it doesn't.
Currently reading: Part 2 of 5
Listen to the audio version here.
Take ACTION here by downloading or making a copy of the TAKE ACTION TOOLKIT: Responding to H.R. 1's Student Loan Changes here.
The Compensation Problem (And Why It's Actually an Opportunity)
Yes, you're right: getting a nursing doctorate doesn't automatically increase your salary. In many traditional employment settings, a DNP or PhD makes zero difference to your paycheck.
And now? H.R. 1 just made this problem significantly worse.
The Student Loan Crisis Nobody's Talking About
Starting July 1, 2026, graduate students will no longer have access to Grad PLUS loans. Instead, there's a $100,000 lifetime borrowing cap for most graduate programs, $200,000 for professional/doctoral programs, and a $257,500 overall aggregate cap across all federal loans.
Translation: DNP and PhD students will graduate with significant debt but fewer options to manage it. The income-driven repayment plans that many of us relied on? Gone. Replaced with only two options: a standard 10-25 year plan, or a new Repayment Assistance Plan that stretches payments over 30 years.
Economic hardship deferments? Eliminated for loans disbursed after July 1, 2027.
So let's connect the dots: You'll take on massive debt to get a doctorate. That doctorate won't automatically increase your salary. You'll have fewer repayment options and less flexibility. And you'll be expected to just... figure it out.
That's the crisis.
And that's exactly why so many doctorally-prepared nurses stay trapped in employment structures that undervalue them, taking whatever salary is offered because they're terrified of their loan payments.
But Here's What Nobody's Teaching You: The Problem Isn't the Credential, It's the Negotiation
The real issue isn't that nursing doctorates don't pay more.
The real issue is that we don't negotiate like we should.
Because here's the uncomfortable truth: others won't value or pay our worth until we do, and until we can clearly communicate it.
When we walk into salary negotiations, contract discussions, or partnership conversations and accept the first offer, or worse, accept an offer out of desperation because of loan payments, we're not just undervaluing ourselves. We're setting the market rate for every doctorally prepared nurse who comes after us.
This is why learning the art of negotiation isn't optional anymore. It's survival.
And it's not just about your paycheck. When you negotiate transparently and successfully, you're negotiating for all of us. You're establishing that DNPs and PhDs bring distinct, valuable expertise that commands appropriate compensation. You're proving that doctoral-level nursing education has a market value.
But when you accept lowball offers out of fear? When you don't ask for more because you're afraid they'll rescind the offer? When you agree to work for exposure, or experience, or the opportunity to "get your foot in the door"?
You're telling employers that doctoral preparation doesn't matter. That they can continue hiring DNPs and PhDs at the same rate as master's-prepared NPs. That our additional training, research capability, systems thinking, and leadership skills have no monetary value.
And that affects every single one of us.
What Negotiation Actually Looks Like for Doctorally-Prepared Nurses
Here's what we need to understand: negotiation isn't about being aggressive or demanding. It's about clearly articulating value and asking for compensation that reflects it.
But most of us have never been taught how to translate our doctoral training into language that employers, clients, or partners actually understand.
And here's something else we need to talk about: you don't have to negotiate for yourself. Having Someone Negotiate On Your Behalf
In many industries, it's standard practice to have someone else negotiate your compensation. Actors have agents. Authors have literary agents. Professional athletes have agents. Executives have headhunters or legal counsel negotiate their contracts.
Why? Because having a third party negotiate protects the working relationship. When your agent asks for more money, the employer doesn't see you as greedy or difficult, they see it as business. The professional relationship starts on day one without the tension that can come from direct salary negotiations.
Nursing has been doing a version of this for centuries, we just call it something else: advocacy.
We advocate for our patients every single day. We negotiate with physicians for pain management. We advocate with insurance companies for coverage. We push back against hospital administrators for safe staffing. We've been collective bargaining through unions for decades.
We know how to advocate. We just haven't been applying it to our own compensation. So who can negotiate on your behalf?
• Staffing agencies or recruiters (they're incentivized to get you higher pay, it increases their commission)
• Professional colleagues or mentors who understand the market and can vouch for your value
• Legal counsel or contract attorneys (especially for high-stakes consulting or academic contracts)
• Business managers or agents (if you're building a substantial consulting or speaking business)
• Your professional organization representatives (in union or collective bargaining contexts)
The key is this: having someone else lead the negotiation doesn't mean you're not involved. You set your non-negotiables, you determine your worth, you approve the final terms. You just don't have to be the one in the room asking for it.
This is especially valuable when:
• You're negotiating with someone you'll have a long-term working relationship with
• You're early in your career and uncomfortable with direct negotiation
• You're from a culture or background where direct negotiation feels inappropriate
• You're carrying trauma from past negative negotiation experiences
• You want to preserve a relationship that matters to you
.png)
What's Actually Negotiable (Almost Everything)
We often think negotiation is just about salary. It's not. Almost everything is negotiable. Consider negotiating:
Compensation:
• Base salary
• Sign-on bonus
• Annual bonus structure
• Profit-sharing or equity (if applicable)
• Productivity bonuses
• Speaking/consulting fees on top of base salary
Benefits:
• Student loan repayment assistance (now permanent under H.R. 1, up to $5,250/year tax free)
• Retirement contributions (employer match %, vesting schedule)
• Health insurance (premium coverage, HSA contributions)
• Continuing education budget
• Professional dues and memberships
• Conference attendance (how many per year, fully funded?)
• Malpractice insurance coverage
Time & Flexibility:
• Start date (negotiate for time between jobs)
• Work schedule (4-day weeks, flex hours, remote options)
• Vacation time (number of weeks, when you can take it)
• CME/conference time (separate from vacation)
• Sabbatical options (for academic positions)
• Protected research/writing time
Professional Development:
• Mentorship structure
• Leadership development programs
• Publishing support (editing, submission fees)
• Research support staff or assistants
• Access to institutional resources (labs, libraries, equipment)
Job Structure:
• Title and credentials on business cards/website
• Scope of practice and autonomy
• Patient panel size or visit expectations
• Administrative vs. clinical time ratio
• Committee or leadership roles
• Intellectual property rights (who owns what you create)
Exit Terms:
• Non-compete clauses (duration, geographic scope, negotiate these down or out)
• Notice period requirements
• Severance package
• What happens to your patients if you leave

What This Sounds Like In Practice
When negotiating employment:
• "I have a DNP degree, which means I've been trained in implementation science and quality improvement. In practical terms, that means when you hire me, you're not just getting a clinician - you're getting someone who can identify why your patient no-show rate is 30%, design an intervention to fix it, and measure whether it worked. That's why my salary expectation is [specific number] rather than the standard NP rate."
When negotiating consulting rates:
• "My doctoral training means I can do more than see patients. I can look at your entire practice, tell you where you're losing money, design a workflow that fixes it, and train your staff to maintain it. That's different from hiring a master's-prepared NP to cover clinic hours, which is why my consulting rate is [specific number] per project."
When negotiating speaking engagements:
• "I've published research on this topic and I teach other nurse practitioners how to implement these strategies in their own practices. My speaking fee is $[X] because attendees don't just get a presentation, they get evidence-based protocols they can use Monday morning, plus my contact information for follow-up questions. That's the difference between hiring an expert versus hiring a speaker."
When negotiating academic positions:
• "I'm bringing an active research agenda on [specific topic], established relationships with [specific funders/collaborators], and a track record of [specific publications/grants]. I'm also carrying $[X] in educational debt with limited repayment flexibility under the new federal loan rules. For me to do this work effectively and sustainably, here's the salary and benefits package I need: [specific numbers]. Let me show you what the return on that investment looks like for your program."
And here's the critical part: you have to be willing to walk away.
Because if you accept an offer that doesn't reflect your value, especially out of desperation because of loan payments, you've just told that employer (and every employer watching) that doctoral preparation can be purchased at a discount.
The Transparency Piece: We're Negotiating for Each Other
This is where it gets strategic.
We need to start talking openly about:
• What we're actually being offered
• What we're actually accepting
• What we're actually asking for
• What successful negotiations look like
Not to brag. Not to make anyone feel bad. But because salary and compensation secrecy only benefits employers.
When you don't know what other DNP or PhD nurses and nurse practitioners are making, you have no baseline for negotiation. When you don't know what successful contracts look like, you don't know what to ask for. When nobody talks about what they turned down or what they negotiated up from, you think the first offer is the only offer.
And employers know this. They're counting on it.
So here's what transparent negotiation looks like in practice:
• Sharing salary ranges in professional groups and networks
• Discussing what benefits and perks are standard vs exceptional
• Being honest about what you accepted and what you wish you'd negotiated differently
• Mentoring newer DNPs and PhDs through their first contract negotiations
• Publishing articles and creating content about compensation expectations
Because when we negotiate in isolation, we negotiate from weakness. When we negotiate with collective knowledge, we negotiate from strength.
The Strategic Response to H.R. 1's Student Loan Changes
Given these new loan limitations and repayment constraints, here's what doctorally-prepared nurses need to do differently:
1. Factor debt into career decisions strategically, not desperately
• Calculate your actual debt load and repayment obligations before accepting positions
• Understand what salary you actually need (not just what you're offered)
• Build a financial plan that doesn't require you to accept the first offer out of panic
2. Leverage employer student loan repayment benefits
• H.R. 1 made employer student loan repayment assistance permanent and inflation adjusted (up to $5,250/year tax-free)
• This should be a standard negotiation point: "Does this position include student loan repayment assistance?"
• If you're building a practice and hiring other NPs, offer this benefit, it's a competitive advantage and it's tax-advantaged
3. Build multiple revenue streams during training
• Don't wait until after graduation to start building your reputation and income sources
• Consulting, writing, speaking, creating educational products, all of this can start while you're still in school
• The goal: graduate with debt, yes, but also with income streams that aren't dependent on a single employer
4. Negotiate like your loans are everyone's problem, because they are
• When you negotiate successfully despite your debt, you prove it can be done
• When you accept lowball offers because you're scared of your loans, you prove to employers that debt makes us desperate
• Your negotiation doesn't just affect you, it affects every doctorally-prepared nurse's market value
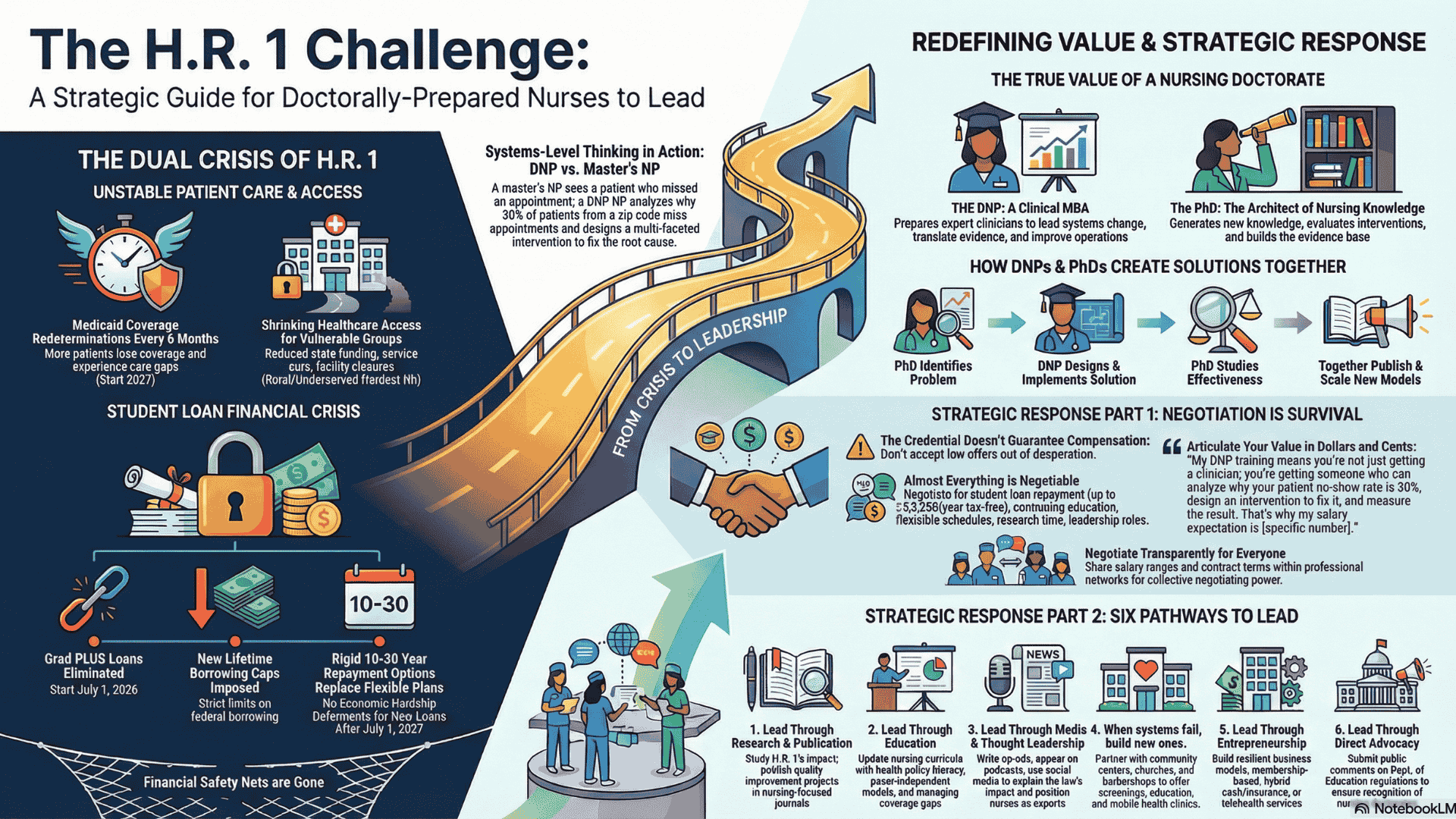
What the Doctorate Actually Gives You
So here's what a nursing doctorate actually gives you, and what you need to negotiate based on:
• The training to see systems-level problems and design solutions (DNP) - Not just "this patient is non-adherent" but "30% of our patients are non-adherent, here's why, and here's the system-level intervention that fixes it"
• The skills to generate evidence and publish your findings (PhD) - Not just "I think this works" but "Here's the peer-reviewed study proving it works, here's the data, and here's the publication that establishes our credibility"
• The credibility to speak on stages, write op-eds, and influence policy (both) - Not just clinical expertise but the publications, credentials, and platform to shape how the profession moves forward
• The expertise to create educational products, consulting services, and thought leadership platforms (both) - Not just working for someone else but building revenue streams from your specialized knowledge
• The authority to train other clinicians and charge accordingly (both) - Not just being a good clinician but being the person other clinicians pay to learn from
• The methodology to evaluate and improve care delivery in ways master's-prepared clinicians can't (both) - Not just delivering care but measuring it, improving it, publishing it, and teaching others to replicate it
That's not clinical work. That's founder work. That's entrepreneur work. That's thought leader work.
And that's what you negotiate for.
The compensation doesn't come from the credential. It comes from understanding what the credential enables you to do, and refusing to accept less than what that's worth.
And with H.R. 1 making educational debt more burdensome and repayment less flexible, we can't afford to keep accepting offers out of desperation.
We need to negotiate like our careers depend on it. Because they do.
And we need to negotiate like every other doctorally-prepared nurse's career depends on it too. Because it does.
Why This Matters Right Now
When systems contract, like they're about to under H.R. 1, the people who can build new systems become invaluable.
Physicians aren't trained for this. They're trained to work within systems. And when those systems fail or disappear? They're often the first ones saying "I can't practice under these conditions."
But doctorally-prepared nurses? We're trained to ask: What system do we need to build so patients can still access care?
That's the entire point of practice doctorates and nursing science doctorates. We don't just deliver care. We design, implement, and study the models that make care delivery possible, especially when traditional structures fail.
So when someone asks "what's the point of a nursing doctorate if it doesn't pay more?"
The answer is: Because we're not trying to get paid more to do the same job. We're trying to build something entirely different.
And that's exactly what this moment requires.
The Real Value Proposition
Here's what DNP and PhD nurses bring to this moment that nobody else does:
DNP graduates bring:
• Systems thinking and implementation science - Translation: "I can figure out why your new protocol isn't working and redesign it so staff will actually use it"
• Quality improvement methodology - Translation: "I can take your patient satisfaction scores from 60% to 85% and document every step so you can replicate it"
• Evidence translation skills - Translation: "I can read 50 research studies, figure out what actually works, and turn it into a protocol your team can implement Monday"
• Leadership training - Translation: "I can lead the team through change without everyone quitting"
• Business and financial acumen - Translation: "I understand P&L statements, payer mix, and how to build a service line that's actually profitable"
• The ability to design care models that work in resource-limited settings - Translation: "I can figure out how to deliver excellent care when you don't have ideal staffing, unlimited budget, or perfect conditions"
PhD graduates bring:
• Research design and methodology - Translation: "I can design a study that will actually answer your question and hold up to scrutiny"
• Theory development - Translation: "I can explain why something works, not just that it works, which means we can adapt it to new situations"
• Program evaluation - Translation: "I can tell you whether your $500K initiative actually did what you thought it would do"
• Grant writing and funding acquisition - Translation: "I can bring in external money to fund the work we want to do"
• The ability to generate evidence where none exists - Translation: "When nobody's studied your specific population or problem, I can design the research and produce the answers"
• Publication and dissemination expertise - Translation: "I can get your work published in peer-reviewed journals and presented at national conferences, which builds your organization's reputation"
Together, DNPs and PhDs can:
• Identify the problem - PhD: "Here's what's actually happening and here's the evidence for why"
• Design the solution - DNP: "Based on that evidence, here's an intervention that will work in your specific setting with your specific constraints"
• Implement it - DNP: "Here's how we roll this out, train staff, handle resistance, and make it sustainable beyond the pilot phase"
• Study it - PhD: "Here's whether it actually worked, for whom, under what conditions, and what we learned"
• Publish it - Both: "Here's the peer-reviewed article that establishes you as a leader in this area"
• Scale it - Both: "Here's the toolkit, training program, and implementation guide so other organizations can replicate your success"
This is the work that fills gaps when policy creates them. This is the work that builds new models when old ones fail. This is the work that ensures patients can still access care when Medicaid coverage becomes unstable and facilities close.
And this is the work physicians aren't trained to do.
So let's stop comparing nursing doctorates to medical degrees and start recognizing them for what they actually are: the training that prepares nurses to lead when systems fail and to build what comes next.
Now let's talk about how.
1. Research Opportunities: Abstracts, Conference Presentations & Publications For PhD Nurses:
This is your moment. H.R. 1 creates a natural experiment in health policy, and we need nurse scientists documenting what happens next.
Priority research questions:
• How does Medicaid coverage instability affect dermatologic outcomes in skin of color populations?
• What are the barriers to early intervention for keloids, CCCA, and acne in populations experiencing coverage gaps?
• How do eligibility redeterminations impact continuity of care for chronic skin conditions?
• What community-based intervention models improve access to dermatologic care when traditional systems contract?
Actionable steps and possible compensation:
• Submit abstracts to the Dermatology Nurses' Association (DNA) Annual Convention and the Society of Dermatology Nurse Practitioners
• Target the National Black Nurses Association (NBNA) and DNPs of Color Annual Conferences for work focused on health equity and skin of color
• Present at Elevate Derm - a conference built by and for advanced practice providers (NPs and PAs) in dermatology and aesthetics, where APP research and clinical innovation are centered (not sidelined)
• Explore American Association of Nurse Practitioners (AANP) National Conference for policy-focused presentations
• Consider poster presentations at interdisciplinary dermatology, tech-focused, and innovation-focused conferences where APP contributions are welcomed
Publish in journals that value nursing science and NP expertise:
• Practical Implementation of Nursing Science (PINS) - A nurse-led, peer-reviewed journal founded by Dr. Kimberly Souffrant, PhD, specifically to bridge the gap between nursing research and practice implementation
• Journal of Cosmetic and Aesthetic Dermatology (JCAD): NP + PA Dermatology Perspectives - Where I serve on the editorial advisory board, focused on advanced practice provider contributions to dermatology
• Journal of Dermatology for Nurse Practitioners and Physician Assistants - Peer reviewed publication centering APP clinical expertise and research
• Journal of the Dermatology Nurses' Association (JDNA) - The established publication for nursing contributions to dermatology
• Journal of the American Association of Nurse Practitioners (JAANP) - For broader NP practice and policy research
• Journal of Advanced Nursing - For theoretical and conceptual work in nursing science
• Health Affairs or Health Services Research - For policy analysis with broader impact
Dr. Kimberly Madison, DNP, AGPCNP-BC, WCC, is a Board-Certified, Doctorally-prepared Nurse Practitioner, educator, and author dedicated to advancing dermatology nursing education and research with an emphasis on skin of color. As the founder of Mahogany Dermatology Nursing | Education | Research™ and the Alliance of Cosmetic Nurse Practitioners™, she expands access to dermatology research, business acumen, and innovation while also leading professional groups and mentoring clinicians. Through her engaging and informative social media content and peer-reviewed research, Dr. Madison empowers nurses and healthcare professionals to excel in dermatology and improve patient care.